Introduction
The circulatory system supplies O2 and substances absorbed from the gastrointestinal tract to the tissues, returns CO2 to the lungs and other products of metabolism to the kidneys, functions in the regulation of body temperature, and distributes hormones and other agents that regulate cell function. The blood, the carrier of these substances, is pumped through a closed system of blood vessels by the heart. From the left ventricle, blood is pumped through the arteries and arterioles to the capillaries, where it equilibrates with the interstitial fluid.
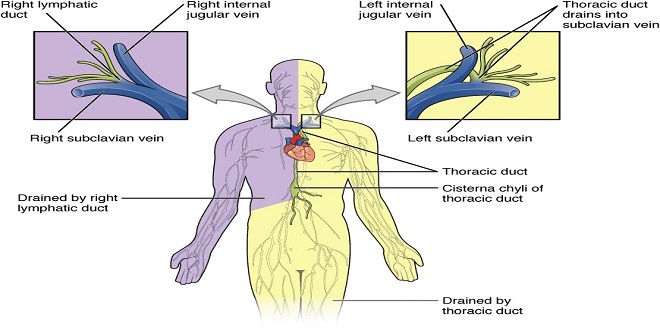
The capillaries drain through venues into the veins and back to the right atrium. Some tissue fluids enter another system of closed vessels, the lymphatics, which drain lymph via the thoracic duct and the right lymphatic duct into the venous system. The circulation is controlled by multiple regulatory systems that function in general to maintain adequate capillary blood flow when possible in all organs but particularly in the heart and brain.
Blood as a circulatory fluid
Blood consists of a protein-rich fluid known as plasma, in which are suspended cellular elements: white blood cells, red blood cells, and platelets. The normal total circulating blood volume is about 8% of the bodyweight (5600 mL in a 70-kg man). About 55% of this volume is plasma.
Read More: Komikli.net
Bone marrow
In the adult, red blood cells, many white blood cells, and platelets are formed in the bone marrow. In the fetus, blood cells are also formed in the liver and spleen, and in adults, such extramedullary hematopoiesis may occur in diseases in which the bone marrow becomes destroyed or fibrosed. In children, blood cells are actively produced in the marrow cavities of all the bones. By age 20, the marrow in the cavities of the long bones, except for the upper humerus and femur, has become inactive. Active cellular marrow is called red marrow; inactive marrow that is infiltrated with fat is called yellow marrow.
WHITE BLOOD CELLS
Normally, human blood contains 4000 to 11,000 white blood cells per microliter. Of these, the granulocytes (polymorphonuclear leukocytes, PMNs) are the most numerous. Young granulocytes have horseshoe-shaped nuclei. That becomes multilobed as the cells grow older.
Role of the spleen
The spleen is an important blood filter that removes aged or abnormal red cells. It also contains many platelets and plays a significant role in the immune system. Abnormal red cells are removed if they are not as flexible as normal red cells and consequently are unable to squeeze through the slits between the endothelial cells that line the splenic sinuses.
Platelets
Platelets are small, granulated bodies that aggregate at sites of vascular injury. They lack nuclei and are 2–4 μm in diameter. There are about 300,000/μL of circulating blood, and they normally have a half-life of about 4 d. The megakaryocytes, giant cells in the bone marrow, form platelets by pinching off bits of cytoplasm and extruding them into the circulation. Between 60% and 75% of the platelets that have been extruded from the bone marrow are in the circulating blood, and the remainder is mostly in the spleen. Splenectomy causes an increase in the platelet count.
Hemoglobin
The red, oxygen-carrying pigment in the red blood cells of vertebrates is hemoglobin, a protein with a molecular weight of 64,450. Hemoglobin is a globular molecule made up of four subunits. Each subunit contains a heme moiety conjugated to a polypeptide. Heme is an iron-containing porphyrin derivative. The polypeptides are referred to collectively as the globin portion of the hemoglobin molecule.
There are two pairs of polypeptides in each hemoglobin molecule. In normal adult human hemoglobin (hemoglobin A), the two polypeptides are called α chains, each of which contains 141 amino acid residues, and β chains, each of which contains 146 amino acid residues. Thus, hemoglobin A is designated α2β2. Not all the hemoglobin in the blood of normal adults is hemoglobin A. About 2.5% of the hemoglobin is hemoglobin A2, in which β chains are replaced by δ chains (α2δ2). The δ chains also contain 146 amino acid residues, but 10 individual residues differ from those in the β chains.
Blood types
The membranes of human red cells contain a variety of blood group antigens, which are also called agglutinogens. The most important and best known of these are the A and B antigens, but there are many more.
The ABO system
The A and B antigens are inherited as mend Elian dominants, and individuals are divided into four major blood types on this basis. Type individuals have the A antigen, type B has the B, type AB has both, and type O has neither. The A and B antigens are complex oligosaccharides that differ in their terminal sugar. An H gene codes for fructose transferees that adds terminal fuses, forming the H antigen that is usually present in individuals of all blood types. Individuals who type A also express a second transferee that catalyzes the placement of a terminal N-acetylgalactosamine on the H antigen, whereas individuals who are type B express a transferee that places terminal galaxies. Individuals who are type AB have both transferees. Individuals who are type O have neither, so the H antigen persists.
Summary
Hypertension is an increase in mean blood pressure that is usually chronic and is common in humans. Hypertension can result in serious health consequences if left untreated. The majority of hypertension is of unknown cause, but several gene mutations underlie rare forms of the disease and are informative about mechanisms that control the dynamics of the circulatory system and its integration with other organs.





